Eligibility verification is the foundation of the home care revenue cycle, accurate, timely checks prevent denied claims, unbillable visits, and revenue loss. Automation streamlines verification, protects cash flow, and ensures compliant, reimbursable care.
Introduction
The home care revenue cycle spanning intake, eligibility verification, authorizations, scheduling, service delivery, documentation, and billing is a chain where every step directly impacts whether an agency gets paid. But none is more critical than eligibility verification, the step that confirms a patient’s active coverage, benefits, and authorization requirements. According to the Centers for Medicare & Medicaid Services (CMS), eligibility and coverage errors remain one of the top drivers of denied or unpaid claims across healthcare settings.
When eligibility checks are rushed, incomplete, or outdated, home care agencies often deliver weeks of care before discovering the patient’s plan changed, benefits expired, or prior authorization was required. Research from university health policy programs such as UCLA Health Policy shows these administrative gaps can lead to significant revenue loss and preventable write-offs.
This article explains why eligibility verification is the foundation of the home care revenue cycle, how poor processes cost agencies thousands each month, and what strategies can protect against avoidable financial loss.
CareVoyant integrates real-time eligibility checks across intake, scheduling, and billing to ensure every visit is reimbursable.
What Is Eligibility Verification in Home Care?
Eligibility verification in home care is the process of confirming a patient’s insurance coverage, benefits, and authorization requirements before services are scheduled or delivered. In home health, home care, private duty nursing, personal care, and therapy services, eligibility ensures that care provided is reimbursable under the patient’s active insurance plan.
A complete eligibility check reviews multiple coverage components, including:
Secondary or tertiary insurance for remaining balances or copays
Medicaid vs. Managed Medicaid plans, which often have different rules, prior authorization needs, and visit limits
Medicare Advantage coverage requirements, which vary by plan
Authorization requirements showing whether services like skilled nursing, therapy, or personal care must be pre-approved
Benefit limits, such as hours per week, units per authorization period, or visit caps
Eligibility is significantly more complex in home care than in hospitals or clinics. Patients frequently switch between Medicaid programs, waiver plans, and managed care organizations; benefits may change monthly; and authorizations are often tied to specific hours or units. This constant variability makes accurate, timely eligibility verification essential for preventing denied claims and unbillable visits.
Why Eligibility Verification Matters in the Home Care Revenue Cycle?
Eligibility verification sits at the center of the home care revenue cycle because every downstream process depends on having accurate, up-to-date payer information. When eligibility is confirmed correctly, agencies can build accurate care plans, ensuring the services ordered are actually covered. It also guides scheduling and staffing, preventing caregivers from being assigned to visits that won’t be reimbursed. Eligibility results determine whether authorizations are required, how many hours or units are approved, and when they must be renewed.
From a financial standpoint, eligibility drives billing and claim submission accuracy. If coverage, benefits, or plan details are wrong at intake, the claim will almost certainly be denied, delaying cash flow and adding costly rework. It also affects reimbursement timelines, since clean eligibility leads to clean claims that are paid faster. According to the Centers for Medicare & Medicaid Services (CMS), missing or inaccurate eligibility documentation is one of the top causes of improper payments in Medicaid and CHIP programs, often resulting in denied or delayed reimbursements.
In home care, eligibility is truly a “garbage in, garbage out” process: one mistake in coverage, plan type, or authorization status can ripple through the entire revenue cycle, resulting in unbillable visits, denied claims, and avoidable write-offs. Proper eligibility verification ensures the agency gets paid for the care it delivers.
The Financial Impact of Poor Eligibility Verification
Poor eligibility verification is a leading cause of revenue leakage, resulting in high denial rates and unbillable caregiver hours.
1. Denied Claims
Eligibility-related denials are among the most common in home care, including codes for inactive coverage, missing prior authorization, or exhausted benefits. Each denial requires staff time to correct, resubmit, or appeal, increasing administrative burden, delaying payment, and driving up AR days.
2. Unbillable Visits & Write-Offs
When eligibility has expired, coverage has terminated, or the wrong plan was billed, visits already delivered become unbillable. Private duty and personal care agencies often absorb 20–50 hours per week of care they cannot bill leading to significant write-offs and caregiver payroll paid without reimbursement.
3. Unauthorized Services
If authorizations aren’t aligned with current eligibility, agencies risk delivering services outside approved units or visit limits. Managed care plans frequently deny these claims, leaving agencies responsible for the cost of care.
4. Missed Secondary Insurance Billing
Failing to verify secondary or coordination of benefits (COB) especially with Medicare/Medicaid crossover patients results in lost revenue that could have been reimbursed at 100%.
5. Increased Administrative Costs
Poor eligibility creates friction between intake, scheduling, clinical, and billing teams. Staff must spend hours calling payers, correcting data, and reconciling mid-episode changes.
6. Compliance Risks
Providing services without verified coverage can trigger payer audits, recoupments, and financial penalties, increasing overall risk exposure.
How Home Care Billing Software Improves Eligibility Verification
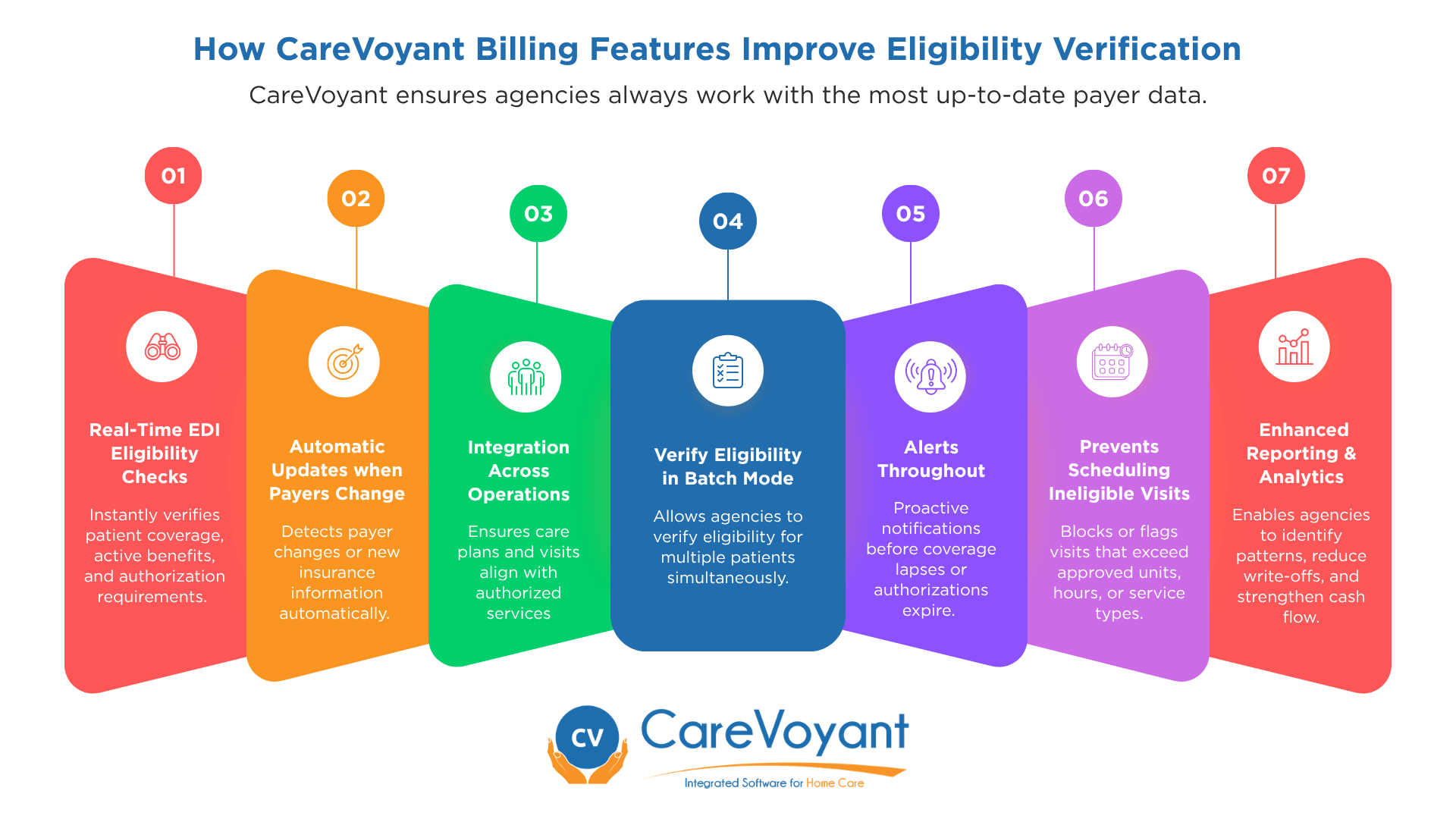
CareVoyant Home Care Billing Software plays a critical role in preventing denials, write-offs, and unbillable visits by automating eligibility checks and integrating them with the entire revenue cycle. The software streamlines billing accuracy by connecting eligibility verification with intake, scheduling, clinical documentation, authorizations, and claims ensuring agencies always work with the most up-to-date payer data.
1. Real-Time EDI Eligibility Checks (270/271)
2. Automatic Updates When Payers Change
Detects payer changes or new insurance information automatically.
Updates patient records in real time to prevent billing errors.
Minimizes risk of unbillable visits due to outdated coverage.
3. Integration Across Intake, Scheduling, Clinical, Authorization & Billing
Eligibility verification is tied directly into every workflow stage.
Ensures care plans and visits align with authorized services by integrating with centralized intake and intelligent scheduling.
Helps maintain accurate documentation for audits and compliance.
Supports smooth coordination between clinical, administrative, and billing teams.
4. Verify Eligibility in Batch Mode
Allows agencies to verify eligibility for multiple patients simultaneously.
Ideal for verifying Medicaid eligibility quickly, managed care renewals, or monthly checks.
Reduces staff workload and ensures all active patients have up-to-date coverage.
5. Alerts for Expiring Eligibility, Benefit Limits & Missing Authorizations
Provides proactive notifications before coverage lapses or authorizations expire.
Supports comprehensive authorization management by tracking benefit utilization.
Helps prevent denials for overutilized or unauthorized services.
6. Prevents Scheduling Ineligible Visits
Blocks or flags visits that exceed approved units, hours, or service types.
Ensures caregivers are only scheduled for reimbursable care, which can help reduce caregiver no-shows by maintaining schedule reliability.
Reduces wasted payroll costs and unbillable service hours.
7. Enhanced Reporting & Analytics
Integrated Reports and Dashboards track denial trends, high-risk payers, unbilled claims, and visit utilization.
Provides actionable insights to improve workflow and optimize revenue.
Enables agencies to identify patterns, reduce write-offs, and strengthen cash flow.
Supports strategic decision-making in authorization management and revenue cycle optimization.
Conclusion
Eligibility verification is the foundation of the home care revenue cycle. When agencies start the care process with accurate, timely, and comprehensive data, every downstream process—from scheduling to clinical documentation—runs more smoothly. Conversely, outdated data puts the entire cycle at risk, leading to denied claims and compliance issues.
Home care organizations that invest in integrated home care software and automation consistently experience fewer denials and faster reimbursements. Real-time verification and automated alerts are no longer just "nice-to-have" features; they are essential for financial sustainability.
If your agency is still relying on manual checks, now is the time to upgrade. CareVoyant Home Care Software provides fully integrated eligibility verification across intake, scheduling, and billing, helping agencies eliminate revenue leakage and optimize their Revenue Cycle Management.
Frequently Asked Questions: Home Care Eligibility Verification
-
Eligibility verification is the process of confirming a patient’s insurance coverage, active benefits, and specific authorization requirements before services are delivered. It ensures that the home care agency will be reimbursed for services provided under the patient's current insurance plan.
-
It is the first "link" in the chain. If eligibility is incorrect, every subsequent step—scheduling, care delivery, and billing—is based on flawed data. Accurate verification at intake prevents the "garbage in, garbage out" effect that leads to denied claims and unbillable visits.
-
The most frequent culprits include:
Inactive Coverage: The patient’s policy was terminated or lapsed.
Missing Prior Authorization: Services were provided without the required payer approval.
Exhausted Benefits: The patient reached their maximum visit or hour limit.
Coordination of Benefits (COB) Issues: Errors in determining whether Medicare, Medicaid, or a commercial plan is the primary payer.
-
While intake is the most critical time, eligibility should be verified at least monthly. Because Medicaid and Managed Care plans can change monthly, and Medicare Advantage plans can update frequently, real-time batch checks are the best way to catch changes before care is delivered.
-
If an agency delivers care that isn't reimbursable due to an eligibility error, they still must pay the caregiver for those hours. This creates "revenue leakage" where payroll expenses go out, but no reimbursement comes in, directly hurting the agency's bottom line.
-
Medicare eligibility usually confirms the "common" benefits and Part A/B status. Medicaid is more complex as patients frequently switch between traditional Medicaid, waiver programs, and Managed Medicaid plans, each with different visit limits and authorization rules that can change every 30 days.
-
These are the standard electronic formats used for eligibility. An EDI 270 is the inquiry sent by the agency to the payer, and the EDI 271 is the response. Automated billing software uses these to provide real-time verification without needing to log into multiple individual payer portals.
-
Batch mode allows an agency to verify the coverage of their entire patient roster simultaneously. This is a massive time-saver for large agencies, allowing them to run a single report to identify any coverage lapses or plan changes across hundreds of patients at once.
-
Yes. Automation eliminates the need for staff to spend hours on hold with insurance companies or manually checking various portals. It allows the intake and billing teams to focus on resolving complex denials rather than performing repetitive data entry.
-
Integrated software like CareVoyant links eligibility directly to the schedule. If a patient’s coverage is inactive or an authorization has expired, the system can automatically flag or block a visit from being scheduled, ensuring that only reimbursable care is provided.
About CareVoyant
CareVoyant is a leading provider of cloud-based integrated enterprise-scale home health care software that can support all home-based services under ONE Software, ONE Patient, and ONE Employee, making it a Single System of Record. We support all home based services, including Home Care, Private Duty Nursing, Private Duty Non-Medical, Home and Community Based Services (HCBS), Home Health, Pediatric Home Care, and Outpatient Therapy at Home.
CareVoyant functions – Intake, Authorization Management, Scheduling, Clinical with Mobile options, eMAR/eTAR, Electronic Visit Verification (EVV), Billing/AR, Secure Messaging, Notification, Reporting, and Dashboards – streamline workflow, meet regulatory requirements, improve quality of care, optimize reimbursement, improve operational efficiency and agency bottom line.
For more information, please visit CareVoyant.com or call us at 1-888-463-6797.
Request for Information
To learn more about CareVoyant Software and how we improve the operational efficiency of Home Healthcare Agencies, contact us: